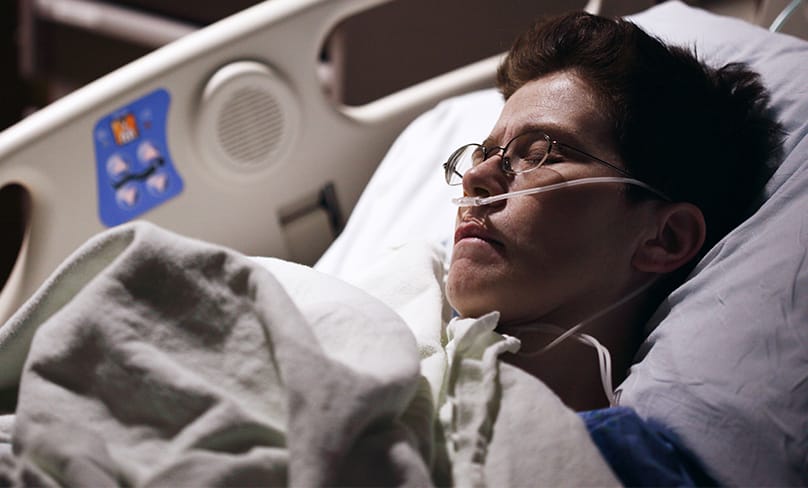
For many doctors and nurses who become palliative care clinicians the decision to devote themselves to end-of-life care comes mid-way through their career.
A junior doctor who sees patients struggling and suffering on the ward can experience a revelation as the palliative care team takes the stage.
A person might change careers and take up palliative care nursing after the experience of seeing a family member with a life-limiting illness bolstered by palliation.
A specialist oncologist who, after years of contact with patients at the end of life, might find the holistic approach of palliative care appealing.
“Your perspective is liberated, or broadened, from the high focus on the physical dimensions of the illness …”
“It’s fascinating, as a doctor, coming into this discipline,” Dr Frank Brennan, one of NSW’s most experienced palliative care doctors, told The Catholic Weekly.
“Your perspective is liberated, or broadened, from the high focus on the physical dimensions of the illness—which is a great skill of doctors, of course.
“But part of the story is beyond that, into the emotional and spiritual dimension of what people are going through.”
Palliative care is essentially an “open” discipline in which clear, compassionate conversations about the realities, fears and possibilities of living with serious illness and death are as important as medical pain relief.

This is part of what attracts a wide range of people to the profession: in a highly-specialised and often bureaucratic medical system, end-of-life conversations may be some of the most human interactions a doctor or nurse could have.
Now that voluntary assisted dying (VAD) is legal in NSW, the situation becomes much more complicated.
“The VAD story will hover over those conversations,” Dr Brennan said.
“That’s one of the many concerns that palliative care has about the introduction of VAD. The response to the suffering of a person starts to be taken over by process.
“The process is a binary—yes, we’ll go to VAD and follow that process, or not—in a way that doesn’t occur without VAD.”
Palliative care clinicians now find themselves in a difficult position.
Palliative Care NSW, the peak body in the state, strongly maintains that palliation and VAD are two separate practices and does not want its people to be expected to deliver VAD once it commences in 18 months.
In the last decade two surveys of members were taken on VAD, with opposition to the scheme dropping from 65% in 2016, prior to the introduction of the defeated 2017 VAD bill, to around 52% prior to the successful Greenwich bill.
Despite the easing of opposition, many palliative care clinicians have conscientious objections to VAD and “will not participate in any way”, Dr Brennan said.
“Most of my colleagues, irrespective of their faith backgrounds—it’s not a faith-based, but a professional response—would be troubled by this.”
So when NSW patients inevitably begin raising the question of ending their lives with their palliative care nurses, doctors and allied health professionals, who are now obliged to provide them information on VAD, what will happen?
“Some people will say, ‘It’s a stain on their reputation as a pal care clinician to even have that sort of conversation’,” said Therese Smeal, a veteran palliative care nurse and President of Palliative Care NSW.
“You can imagine that if you were to be seen either very pro- or very anti-VAD, for particular patients or families that could be very disconcerting to say the least.”
“Others will maybe be more like me, feel like there shouldn’t be any conversation that’s off limits with our patients and family.
“Then you’d just need to guide them as to who they need to go to, to further investigate that.”
Ms Smeal said Palliative Care NSW, as a peak body that represents but does not employ palliative care clinicians, was taking a neutral stand towards the new legislation.
“You can imagine that if you were to be seen either very pro- or very anti-VAD, for particular patients or families that could be very disconcerting to say the least, depending on what their wishes may be,” she said.
Neutrality is also a response to the complex range of views toward VAD among the palliative care workforce.
While the official position of peak bodies is that palliative care and euthanasia are separate disciplines, a small number of clinicians who have no objection to VAD personally see them as two choices within the same end-of-life situation.
In Victoria, a handful of palliative care clinicians are already offering VAD.
To further complicate the question, some who find VAD objectionable may nevertheless see it as the lesser of two evils for it to be offered within the context of palliative care.
They are put in the difficult position of knowing that end-of-life conversations that begin with high emotion, with patients who may feel they need VAD because they “can’t go on any longer”, often have roots in anticipatory grief, worries of becoming a burden, and fear of loss of autonomy—all these require time and effort to unfold.
But as case studies from Canada and other jurisdictions show, medicos within the context of routinised hospital systems will inevitably respond to some requests for VAD with a promise to “get the forms”.
“There aren’t many people in health who are great communicators around end-of-life issues,” Ms Smeal said.
“I include in that surgeons, geriatricians, etc. For all these people who are caring for people who die day in, day out, (and I’m being very generalised here) they are often very poor communicators.
“You don’t have to be a Rhodes Scholar in psychology to have those conversations.
“What you have to do is put your big girl undies on and be prepared to sit in that presence of that person, and hear the difficult conversations, realise you don’t have to offer solutions, but enable those people to talk about what are often their most intimate things, concerns etc.”
There are also concerns among palliative carers that VAD drugs do not always work. Without medical or nursing staff present, this can be a disaster.
“People don’t know, and why should they know?” said Linda Hansen, CEO of Palliative Care NSW.
“You might throw everything up, have a horrible episode, your organs are in a horrible state. Not often – I’m not trying to dramatise it – but things go wrong.”
For staff in nursing homes, discovering the body of a resident who has died from VAD (patients are not obliged under the new laws to notify nursing home staff) or who has administered the drugs and survived, could be a distressing experience.
“That’s why some palliative care people will be a part of it, even if they don’t necessarily agree with it, because they don’t want to see that situation,” Ms Hansen said.
Making head and tail of this highly-charged and complex situation, involving issues of care, conscience, life and death, will require clarity from the NSW Government on palliative carers’ obligations under the new laws.
Ms Hansen says the NSW Government must make sure that people who work in the health sector are respected, “whatever their views are”.

The sector, despite having had more funding support from the NSW Government in recent years, operates mostly on 3-4 year funding blocks.
With an extra layer of complexity around VAD, palliative care is desperate for more security.
The leadership of Palliative Care NSW also hope that now the debate is over, the “inflammatory” language used by advocates of VAD will cease.
They are feeling bruised and misrepresented by high-profile VAD advocates in parliament and the media, who have caricatured terminal illness and end-of-life care in “a very selfish approach to get their cause”, according to Ms Smeal.
“If access to palliative care were more widespread, the ‘horror stories’ relayed during the debate simply would not have occurred in most cases.”
“At one stage we pleaded very strongly with the group that had carriage of the legislation,” she said.
“‘Yes, yes. We understand, we will.’
“In 12 hours you’re hearing them again using that same language.”
She said that terminally ill patients and their families under palliation have been distressed by the debate.
“If you’re a person who’s got stage four lung cancer with a prognosis of 2-3 months, and you flick on the news and there’s a politician waxing lyrical about horrendous death – people choke to death, suffocate to death, this or that – that’s been the disappointing part of the debate.”
If access to palliative care were more widespread, the “horror stories” relayed during the debate simply would not have occurred in most cases – a source of frustration for the sector, which is desperate for more funding, more support, and recognition by Australia’s “death defying” culture.
“We’re past all of that now, let’s move on and see how we can reshape palliative care moving forward,” Ms Hansen said.
“A lot of that is empowering people who work in pal care. We don’t have the resources, but we’ll try.”
