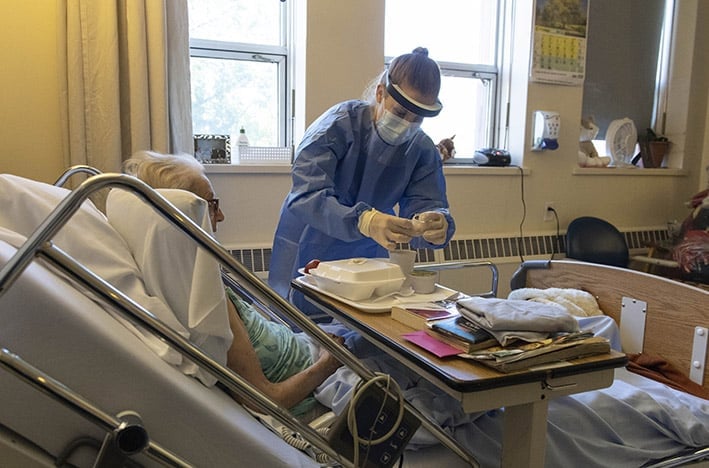
The “ethical tone” of a society is not determined by how it treats its most powerful, strongest, most affluent members, but by how it treats its weakest, most in need, most vulnerable members. The latter include elderly persons in some aged care institutions. What does our appalling treatment of them, in particular in the COVID-19 pandemic, tell us about ourselves and the “ethical tone” of our contemporary Australian society?
Basic presumptions
Basic presumptions are important in ethical decision-making, because they reflect our values and biases, influence our decisions about what is and is not ethical, and when we are in a situation of equal doubt about what we should do, the basic presumption governs.
For example, let us imagine we are torn in deciding whether an old person in an aged care institution, who is seriously ill with COVID -19, should be admitted to hospital. If our basic presumption is “yes, hospital treatment should be provided, but not if …”, the person will be admitted to hospital unless those arguing against this establish that the conditions for not doing so are fulfilled. Note these conditions must be ethically acceptable so must not include age discrimination. In contrast, if our basic presumption is “no, hospital treatment should not be provided, unless…” then, in exactly the same circumstances, the person will not receive treatment unless the person arguing for treatment can prove the conditions for providing it are fulfilled.
Saturday morning on ABC TV Chanel 24, an ABC journalist reported doctors as saying Melbourne hospitals were full, because people with COVID-19 were being transferred from Aged Care homes and that meant other people presenting at Emergency were experiencing serious and unacceptable delays, in one case 60 hours, and beds needed for them were not available. The journalist seemed to be employing a basic presumption that the latter category of patients should have priority for hospitalisation over the elderly people. The same presumption probably underlies the directive that aged care residents with COVID-19 must not be transferred to hospital, issued by NSW Chief Health Officer Dr Kerry Chant to Anglicare’s Newmarch House, where at least 17 residents died of COVID-19.
Belgium presents a striking case of such an approach. At the beginning of the pandemic approximately two thirds of people who died from COVID-19, the vast majority of whom were elderly, died in hospital. Now only around 14 percent do so. I have tried to ascertain how many Belgian COVID-19 deaths are by euthanasia, but was unable to do so.

The absence of that information is also true for Victoria in relation to its Voluntary Assisted Dying (VAD). Médecins Sans Frontières – Doctors Without Borders have released a report that included surveying the mental health of people in aged care homes in Belgium and found that their consideration of resorting to euthanasia had increased.
Left behind in the times of COVID-19 report
Reports of elderly residents of aged care facilities with COVID-19 being sedated with morphine and other drugs have emerged and the ethical concern here is twofold.
Sedation as a form of “chemical restraint” or “behaviour control” is uniformly condemned as unethical. Many aged care facilities are understaffed, whether chronically or because of COVID-19, and, moreover, lack sufficient or even any healthcare professionals on staff.
This lack can also link to an unethical failure to transfer seriously ill residents to hospital. A doctor or nurse must authorise the transfer before ambulance attendants will comply. Sometimes systems are intentionally established in such a way as to hinder attribution of responsibility for breaches of ethics. To avoid unethical or negligent systems, we must expressly embed ethics in the system.
As well, the use of sedation at the end-of-life is very ethically sensitive. When sedation is the only reasonable way to relieve serious suffering, appropriate drugs and doses are used, and there is no primary intention to shorten life, it is ethically acceptable palliative care – “palliative sedation”. When sedation does not fulfil those conditions and is used as a form of so-called “terminal sedation”, it is “slow euthanasia” and ethically unacceptable. The latter use is increasingly common in Belgium and the Netherlands. One explanation for its dramatically expanded use is that it is less psychologically traumatic for doctors than administering euthanasia by lethal injections.
A “world of competing sorrows”
The situations described above are examples of what we call in Bioethics a “world of competing sorrows”: there are no, “no harm” options and we must choose who will suffer the harm. There are, however, some principles that can guide us in these situations. Our obligations include a preferential option in favour of the weakest, most in need, most vulnerable people. Another, is that those who suffer the burdens should have access to the benefits that result. This can mean that healthcare professionals should have priority access to any treatments or preventive measures, which are discovered and, likewise, volunteers for COVID-19 research. It also means that as a community or society we have obligations to reduce to the lowest possible level the risks people take to care for people with COVID -19. It is appalling that in some hospitals or aged care institutions staff have inadequate Personal Protective Equipment (PPE).
As Shakespeare said, “the primrose path to the everlasting bonfire is paved with good intentions”. We are trying to protect people from COVID-19 with lockdowns, but they are losing their jobs and capacity to support their families, as well as suffering the mental trauma that involves. We are all in the COVID-19 crisis together, but some of us are much more vulnerable than others of us. We must also consider the breaches of human rights that preventive measure can involve, such as loss of liberty and freedom of assembly.
Ethics at different levels of decision-making and action
There are four levels of ethical decision-making and action resulting from the decisions taken. They can only be briefly identified here, but all are relevant to dealing ethically with COVID-19.
Micro or individual level: What do I owe to others to keep them safe and what do others owe to me to keep me safe? In the doctor–patient relationship, the doctor has a primary obligation of personal care to the individual patient – their “best interests” must come first, which can require being a patient advocate for an elderly person.
Meso or institutional level: The ethical principles and considerations, which should govern aged care institutions, involve organisational, institutional and systems ethics. Ethics preparedness, including for a pandemic, is an ethical requirement.
Just following institutional policies or guidelines does not automatically mean we are acting ethically. Indeed, some policies or guidelines can be unethical, for example, those that breach human rights because they discriminate on the basis of age or disability.
Unlike at the individual level, effectiveness and efficiency in the use of healthcare resources, and justice, are ethically valid primary considerations at this level. We cannot have, however, a blanket rule, e.g. of refusal of treatment for certain people. We must also, at the least, consider each person’s claims and needs on their merits. In this context, as explained already, the choice of a basic presumption is important.
Legally, civil or criminal liability can arise from a failure to provide medical care. There are legal duties to provide the necessaries of life – which include basic hygiene and medical care, and food – to a person in one’s care custody or control, who is unable to provide them for themselves. Wanton and reckless indifference to human life or safety and medical negligence (medical malpractice) are also relevant considerations.
Macro or societal level: Ethical issues include hyper-bureaucratization of Public Health officials’ decisions; politicians politicizing issues, as compared with sound health and social policy decision making; politically or ideologically driven intolerance; failure to remedy socio-economic disparities in health status or to provide support for the most vulnerable people; and so on.
Public Health’s mandate of avoiding danger to citizens and ensuring their safety is an exercise of the state’s police power, which is much broader and coercive than its parens patriae power, which is to protect those unable to protect themselves, although both powers – and their concomitant obligations – are relevant to fulfilling the justified claims of elderly persons.
Mega or global level: Ethical issues include principles governing research on a vaccine and access to a vaccine when available; the use of tissue from intentionally aborted foetuses to manufacture a vaccine; medical research in developing countries – those who bear the burdens should have preferential access to the benefits; fraudulent research, for example, regarding hydroxchloroquine as a treatment for or protection from COVID-19 ; protective equipment for healthcare workers; media ethics in reporting on the pandemic; and so on.
Overlap among the levels: Take, for example, issues relating to elderly persons. They arise at more than one level and include elderly persons’ rights to protection and access to care; respect for the dignity of the person; balancing aged care institutions’ obligations to each resident and to all residents; government responsibility for funding aged care and for persons with disabilities; and so on.
Ethics responsibility is not like a football, in that one person can divest them self of it by throwing it to another person. This approach was manifest among people involved in the decision to let COVID-19 infected passengers on the Ruby Princess cruise ship disembark in Sydney, quickly trying to pass the blame on to someone else. Rather ethics responsibility is like a cake, everyone can have a slice.
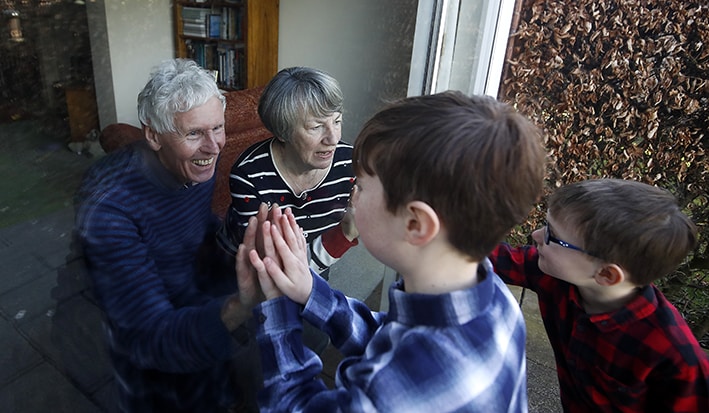
Social capital
Finally, for this article (there are a legion of other ethical issues or dilemmas raised by COVID-19 not addressed herein), whether the pandemic will increase or decrease social capital is an important consideration. Philosopher Robert Putnam describes “social capital” as the “features of social organization such as networks, norms, and social trust that facilitate coordination and cooperation for mutual benefit.” A major question is will how we deal with COVID-19, as individuals, families, communities, state societies and an Australian society, increase or decrease our social capital? Our actions and responses are highly unlikely to be neutral in that regard; they will do either one or the other.
Questions we need to address include what are the roles and responsibilities of all of us in maintaining and creating social capital, not just for our own benefit but also for the good of society in general. What about specific groups such as doctors and other healthcare professionals or teachers? And what about institutions? Hospitals and the healthcare system? The Legal System? Industry? Banks? Financial Institutions? Universities? Governments? And what about workers in everyday activities, for example, supermarkets, garbage collection? In the future, COVID-19 might be seen looking back, as having been a dramatic wake-up call regarding our obligations regarding “social capital”. We should heed it if we want to pass on to future generations societies in which reasonable people would want to live.
Conclusion
Overall, Australia has done well in managing the COVID-19 pandemic, but not in Aged Care, where the Aged Care Royal Commission has been told 68 percent of Australia’s COVID-19 deaths have occurred, the second highest rate of death in residential aged care from COVID in the world. We need to ask ourselves why this is.
A partial explanation is that older people face a greater risk of death from the virus. Another important reason, however, is rampant ageism in Australia – wrongful discrimination against elderly persons. The collision of two pandemics – COVID-19 and ageism – is indeed lethal. We do not respect elderly people or their human dignity – our Aboriginal brothers and sisters are an exception and we other Australians have much to learn from them in this regard. Sometimes, this failure of respect is subtle, for example, a panellist on ABC TV’s The Insiders pointed out that the media is speaking of aged care residents being “decanted” to hospitals: we decant wine and other things, not persons. Words matter and nowhere more so than in ethics decision-making.
People are supporting legalised euthanasia, because they would rather be dead than admitted to an aged care residence. In the context of COVID-19, heart-breaking footage of desperate elderly people trying to communicate with their loved ones through locked windows should spur us to instant remedial action. We all justly fear dying alone.
Margaret Somerville is Professor of Bioethics in the School of Medicine and the Institute for Society and Ethics at the University of Notre Dame Australia
Related
Margaret Somerville: Withdrawing artificial hydration and nutrition
Euthanasia ‘like a new pandemic’
