
Catholic hospitals say ‘no patient will be left behind’
Disability and pro-life advocates and faith leaders are concerned at signs that some of the people most vulnerable to COVID-19 may be triaged out of life-saving treatment. But the Catholic health care sector is adamant that “no patient will be left behind”.
The recent discovery of a Perth grandmother that she had been assigned a ‘do not resuscitate’ order against her wishes when she was hospitalised with the virus is troubling, says director of HOPE Branka van der Linden.
“Our concern is that the elderly and people with disabilities or those living with chronic illnesses already feel judged about their quality of life,” Ms van der Linden told The Catholic Weekly.
“Add into the mix a rationing of medical and health resources because of the coronavirus, and suddenly vulnerable people can feel especially at risk of doctors making value judgments about whether they are ‘deserving’ of life-saving treatment, or whether these should be allocated to someone younger or healthier or without disabilities.”
The Royal Commission into Violence, Abuse, Neglect and Exploitation of People with Disability has also addressed the problem, calling on Australian governments to ensure that responses to COVID-19 include dedicated strategies and take the necessary measures to protect and support people with disability.

In a statement of concern it said that one of the main worries it had heard from people with a disability is that “discrimination or unconscious bias could impact their access to critical and lifesaving health care during this crisis”.
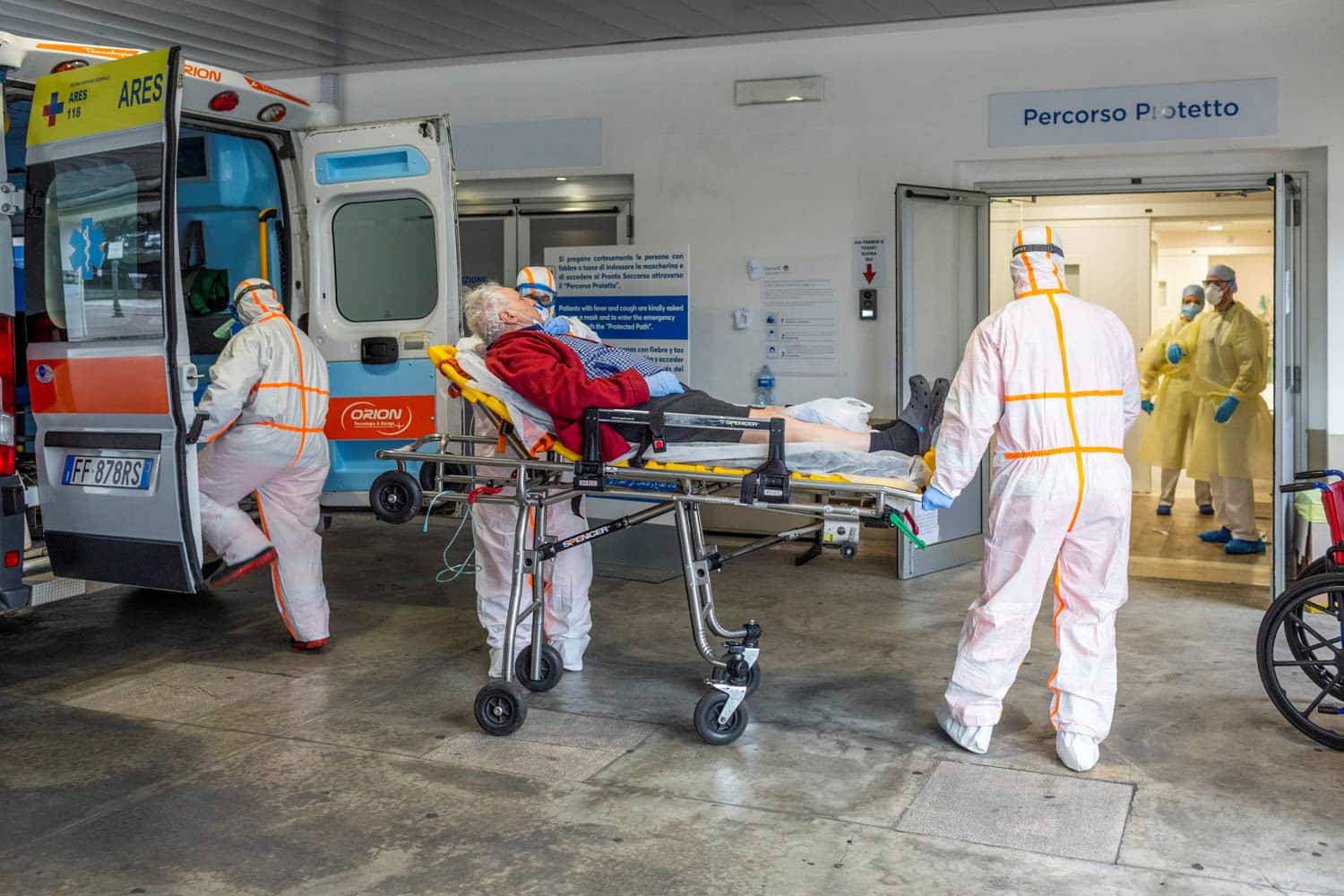
Lorraine Lewis, 71, contracted the virus in Italy. Upon returning to Perth was admitted to the Sir Charles Gairdner Hospital and asked if she wanted a ‘do not resuscitate’ instruction if her condition worsened. She declined, but was later shocked to find her discharge papers said that she did not want CPR, ICU or intubation.
Ms Lewis told media last week that she assumed the decision was made on her behalf because she had been classified as elderly. “It’s so wrong,” she said. “I don’t care how old that person is, they’ve got a right [to treatment].”
Ms van der Linden said she is not surprised if people with disabilities “who do not have strong advocates fighting for them would be feeling especially vulnerable in this current climate”. “The reality is that every person has value and is deserving of society’s care and resources, no matter what,” she said. “Our health systems must reflect and adhere to this basic principle of equality and human worth.”
Chief executive officer of Catholic Health Australia Pat Garcia said that caregivers, patients, their families and the Australian people can be reassured that “we remain steadfastly committed to our ethic of compassionate care for all”.
“We care for, accompany and never abandon any person, regardless of their condition, to the best of our ability and resources,” Mr Garcia said. “Catholic hospitals are particularly attentive to social disadvantages which can compound the medical needs of vulnerable individuals and groups.
“Catholic health care will always seek to serve and be advocates for those at the margins of society who are especially vulnerable to discrimination.” Group manager of ethics and formation at St Vincents Health Australia Dr Dan Fleming said that across its network “extensive preparations” have been made to ready its services in case of a surge of hospital patients.
“I don’t care how old that person is, they’ve got a right [to treatment].” Ms Lewis
“If allocation of scarce resources (such as ICU beds) becomes necessary, our staff will base it on patient need, prognosis, and the prospect of success for therapy,” he said. “It will be based on whether the treatment is therapeutic. “Determining this looks to all aspects of a patient’s condition and is never a case of employing crude exclusions on the basis of age, background or any other personal attribute.
“We have a sophisticated system in place, which includes the establishment of triaging teams, to consider these kinds of questions if they arise. “Importantly, we have also been doing a significant amount of preparation work to ensure that there are care pathways available for all patients who come to us.
“Every patient will be cared for, and no patient will be left behind.” A recent report by the Center for Public Integrity in the United States found that 25 out of 30 states with policies and guidelines about the rationing of ventilators had “provisions of the sort advocates fear will send people with disabilities to the back of the line for life-saving treatment”.

“These policies take into account — in ways that disability advocates say are inappropriate — patients’ expected lifespan; need for resources, such as home oxygen; or specific diagnoses, such as dementia,” it said. “Some even permit hospitals to take ventilators away from patients who use them as breathing aids in everyday life and give them to other patients.”
The Catholic bishops of Mexico and England said that while tough triage decisions must be made because of the pandemic, age should not be the only criteria for deciding which patients receive treatment.
The Mexican bishops’ conference issued on 16 April ethical guidelines as medical staff in the country are potentially forced to make life-and-death decisions on who will receive treatment. Similarly, the bishops of England and Wales on 20 April pleaded for fairness in the possible rationing of health care to coronavirus patients amid rising fears that protective and life-saving equipment is running out.
Bishop Richard Umbers, a member of the Bishops Commission for Life, Family and Public Engagement, said that a society “grounded on usefulness to the economy and pleasure, rather than on the dignity of all, will generate these kinds of abuses”. “By their fruits, you will know them,” he said.
Back in Perth, a statement from the Sir Charles Gairdner Hospital apologising to Ms Lewis simply read that: “The clinician documented that Ms Lewis was accepting of the proposed course of action, when she may not have been at the time”.
Related articles:
Catholic healthcare workers on the COVID-19 frontline
Catholic hospitals join pandemic fight
Ethics for Australian healthcare in the midst of a pandemic

