
Euthanasia and voluntary assisted dying (VAD) poses the risk of disruption and intrusion to the practice of palliative care, leaving palliative carers distressed, disempowered and under pressure, the immediate past president of the (ANZSPM) has said.
In answers to supplementary questions from the NSW Voluntary Assisted Dying bill inquiry, Professor Leeroy William said that in Victoria, where euthanasia is legal, “VAD has disrupted the necessary teamwork and inter-professional relationships to deliver and sustain optimal end-of-life care”
“Clinicians have been caught between legal, professional and personal positions that have divided opinions about optimal end of life care.”
Palliative care and euthanasia/VAD are often considered part of the same end-of-life process, but both palliative care clinicians and the Royal Australasian College of Physicians (RACP) insist the two must remain separate.
“Voluntary assisted dying must not be seen as part of palliative care,” the RACP said in a 2018 paper.
“Across the healthcare system, standard medical practices have been neglected to ensure the legislative requirements are upheld.”
Professor William told The Catholic Weekly that in his role as immediate past president of the ANZSPM he “was able to listen to the many concerns of palliative care clinicians” about the intrusion of euthanasia/VAD into palliative care practices.
“Across the healthcare system, standard medical practices have been neglected to ensure the legislative requirements are upheld,” he said.
“For example, a request for information about VAD can trigger a process of referral rather than the usual conversation to explore the reasons behind the request.”
Professor William provided case studies to the inquiry, which were de-personalised to protect the confidentiality of both doctors and patients.
COVID-19 has also disrupted the ability of palliative care clinicians in Victoria to share their experiences directly.
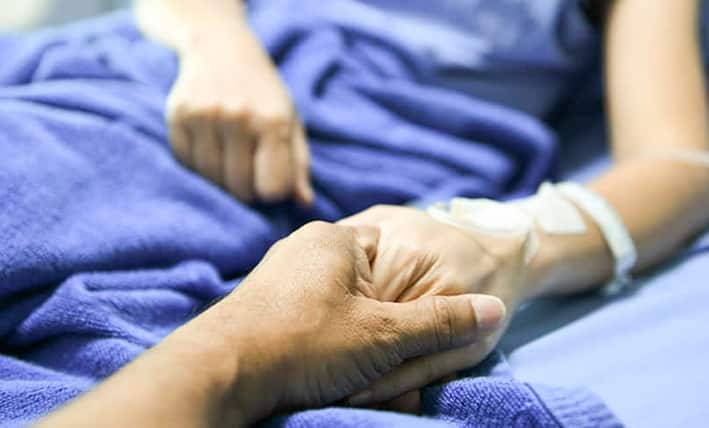
In one case study, a hospital patient requested VAD on a palliative care unit and a transfer to another ward was organised.
Although “[t]he treating teams respected the need to keep VAD and palliative care separate … The hospital over-ruled the clinicians and the patient had VAD on the palliative care unit”.
“Staff were distressed and the clinicians felt disempowered in their roles,” the case study in Professor William’s submission said.
A second case study reported that care clinicians “have felt pressured to deliver VAD on their units, despite the RACP position. They have felt uncomfortable about their potential facilitation in the VAD process”.
“Staff on the ward felt uncomfortable about VAD occurring on their ward and the possible stigmatisation of their ward in the future,” a third case study reported.
“Many patients have enquired or requested VAD to avoid transfer into a residential aged care facility.”
A fourth said that elderly patients are particularly affected by euthanasia, reporting that “Many patients have enquired or requested VAD to avoid transfer into a residential aged care facility.”
Professor William told The Catholic Weekly that the intrusion of euthanasia/VAD into palliative care depends on three factors.
“Firstly, the perceptions regarding what palliative care does and the expectations on these services to provide VAD.
“Secondly, how palliative care services can change or withstand the misperceptions and pressures that will exist.
“And finally, palliative care services need to clearly distinguish and work within the bounds of the moral and clinical practice of palliative care to ensure there is no conflation with VAD.

“In practice, keeping palliative care service and VAD separate is challenging, especially in the home setting.”
Misconceptions around end-of-life care often confuse or conflate accepted practices of palliation, such as “withdrawing or withholding treatments” with euthanasia, which involves the administration of lethal doses of drugs.
Labor MLC Greg Donnelly said Professor William’s evidence was “significant”.
“The case studies should not be a surprise to anybody. They capture circumstances that are not unusual and can be easily imagined.
“It is clear that this is an issue with strong and passionate opinions, which are felt deeply by both sides of the debate.”
“In fact it is these very circumstances that make the case studies so concerning.”
The NSW Legislative Council’s inquiry into independent MLA Alex Greenwich’s VAD laws published its report in late February, but did not take a position on the bill.
“It is clear that this is an issue with strong and passionate opinions, which are felt deeply by both sides of the debate,” Committee chair Wes Fang MLC wrote in the report’s foreword.
“Further, it is also clear there is no consensus amongst stakeholders as to the merits of the bill. Indeed, there was no consensus amongst the committee members themselves.”
The bill will continue to be debated in NSW Parliament when it returns on 22 March.
